
Results of a 32-year-old female nulliparous patient The body mass index
Download scientific diagram | Results of a 32-year-old female nulliparous patient The body mass index of the patient was 20.4 kg/m 2. The oncologic breast surgeon performed skin-sparing mastectomy. (A) Preoperative view. (B) Postoperative view at 6 months of follow-up. (C) Postoperative view at 12 months after nipple reconstruction. from publication: Weight analysis of mastectomy specimens and abdominal flaps used for breast reconstruction in Koreans | Background: Slim patients or those with large breasts may be ineligible for breast reconstruction with an abdominal flap, as the volume of the flap may be insufficient. This study aimed to establish that abdominal tissue-based breast reconstruction can be well suited for | Breast Reconstruction, Mammaplasty and Free Tissue Flaps | ResearchGate, the professional network for scientists.

Associations of Gestational Perfluoroalkyl Substances Exposure with Early Childhood BMI z-Scores and Risk of Overweight/Obesity: Results from the ECHO Cohorts, Environmental Health Perspectives

Baseline characteristics and pregnancy outcomes of the study
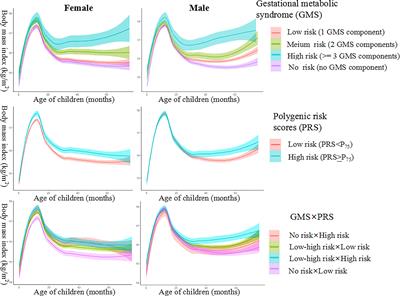
Frontiers Sex Discrepancy Observed for Gestational Metabolic Syndrome Parameters and Polygenic Risk Associated With Preschoolers' BMI Growth Trajectory: The Ma'anshan Birth Cohort Study

Standards for Professional Registered Nurse Staffing for Perinatal Units - Nursing for Women's Health
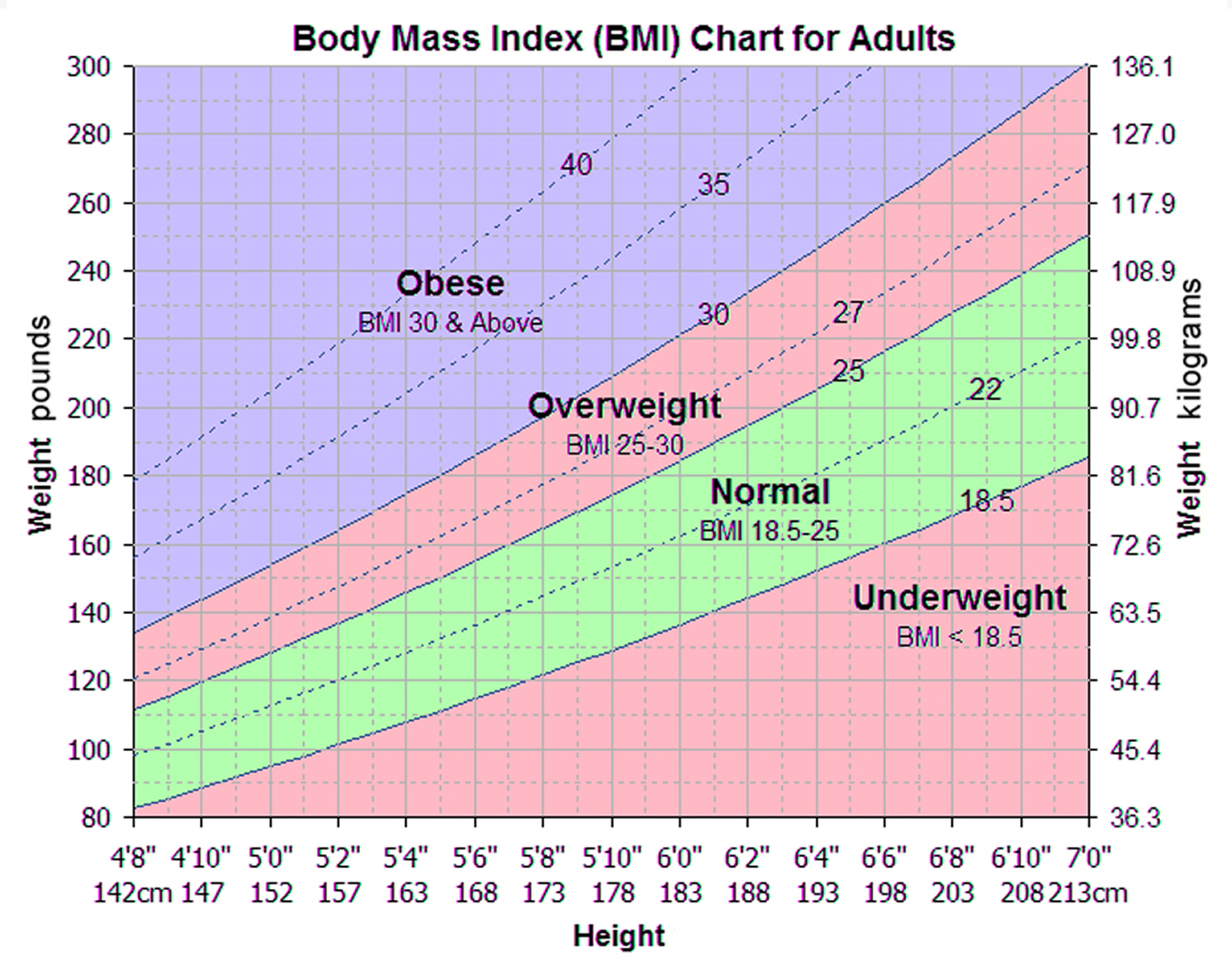
Body Mass Index Chart, Formula, How To Calculate for Men & Women
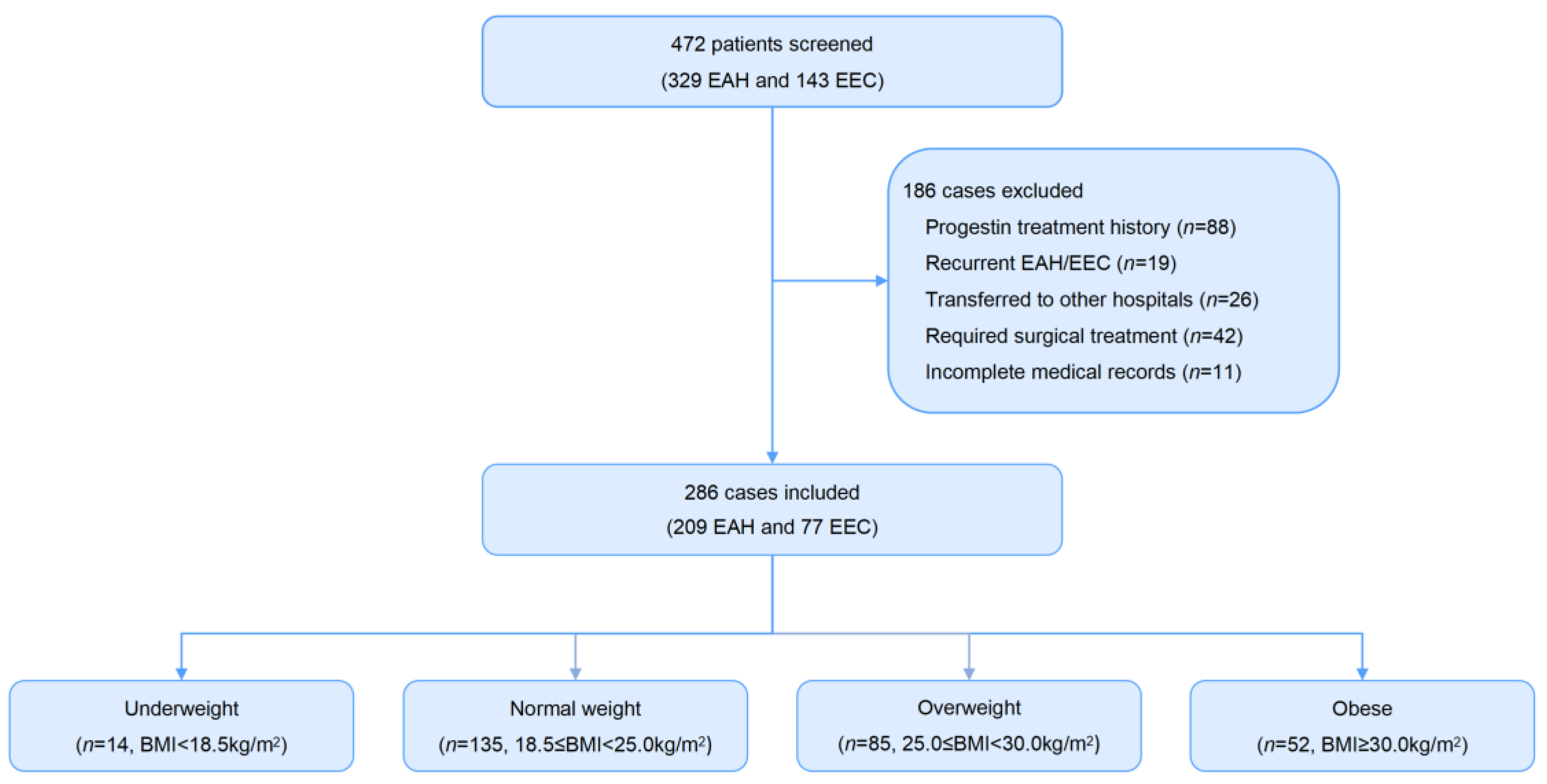
Cancers, Free Full-Text
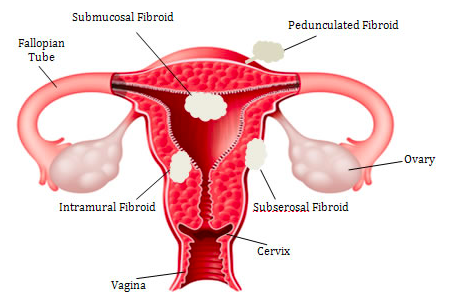
NBME OBGYN Form 4 – Step Prep

Hyung Hwa Jeong's research works University of Ulsan, Ulsan (UOU) and other places

Effect of Body Mass Index on pregnancy outcomes in nulliparous women delivering singleton babies, BMC Public Health

Maternal prepregnancy body mass index and risk of bronchopulmonary dysplasia

a Preoperative anterior–posterior view of a 20-year-old single and

assessment of the female genitalia

Body mass index (BMI) distribution in severely obese and comparison
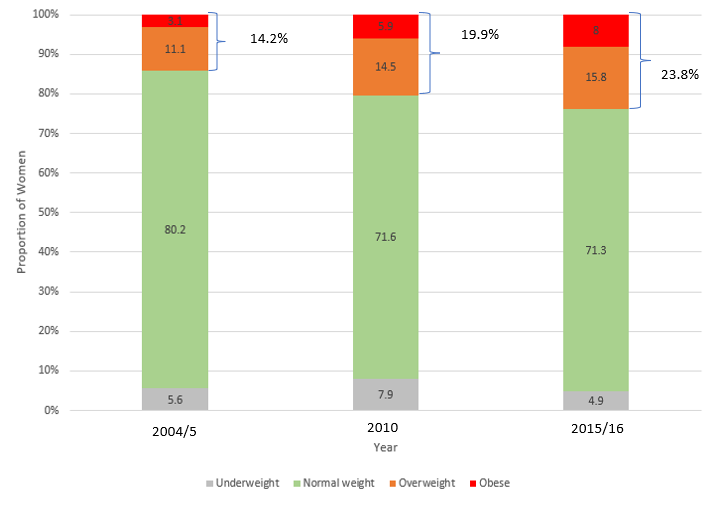
Increasing prevalence of overweight and obesity among Tanzanian women of reproductive age intending to conceive: evidence from three Demographic Health Surveys, 2004-2016





.jpg)
